As debate continues over whether it is acceptable that for some women having the coil fitted remains a painful and traumatic experience, two women share their experiences.
When it comes to pain and discomfort around certain health issues, sadly, particularly for Black women, the expectation is to just grin and bear it, the greatest of these being over childbirth. However recently, more people are challenging the narrative that pain in healthcare is inevitable and holding health care providers to account.
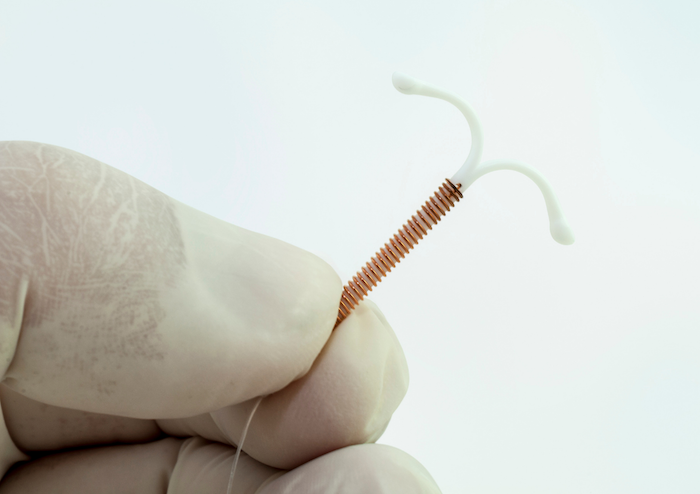
In recent weeks, the coil (Intra Uterine Devices), which can be used as a contraception or for regulating heavy periods has been in the spotlight. BBC Radio 5 Live presenter Naga Munchetty set the conversation ablaze with her account of passing out from the pain twice during her fitting. She was motivated to speak out after a Caitlin Moran article challenged the “grin and bear it” narrative around female reproductive health.
While some women sing the coil’s praises, saying it was the only option for them and their fitting was a breeze, too many describe a process of excruciating pain and being ill-prepared for the experience by their GP or nurse.
With data showing that Black women do not benefit from the same level of patient advocacy and pain management as their white counterparts, we spoke with two Black women who shared their experiences.
*Zara: Early 40s. West Indian. Lives in the Midlands.
“My first fitting with the Mirena Coil was in 2009. It was to help with my Polycystic Ovary Syndrome. It was done by a male consultant in Nottingham who did not explain the procedure well at all. I had an awful time with it. Cramps, lots of blood and general discomfort.
He just wasn’t attentive, and I already had gynaecological issues so his attitude didn’t put me at ease. Funnily enough, I did some of my own research after that fitting and eventually asked a female doctor who specialised in women’s health about my pain. Her immediate response was “that’s not right, get it taken out.” The young male GP I saw after I’d endured debilitating cramps and excessive bleeding immediately set up an appointment to have it removed. This time, I was listened to. I grant you, that coil may have shifted, which caused the extended pain. But still, I found my needs were better met when the procedure was done by someone attached to my GP’s surgery – someone who was familiar with my history. That coil was removed in 2012.
“My screams were so loud that my husband tried to find out what room I was in to make it stop.”@TVNaga01 tells her listeners about “one of the most traumatic physical experiences” she has ever had.
📻 @BBCSounds – https://t.co/7lXKKAi7px pic.twitter.com/Tr117sOyzx
— BBC Radio 5 Live (@bbc5live) June 21, 2021
Years later I had another one fitted. The procedure to insert was very painful and the nurse didn’t even want to continue. She had to do all sorts of things to get me open enough to fit it. I remember afterward I had to find somewhere quiet to lie down for hours to avoid passing out. The pain was that bad. The one I have now has given me no trouble.
I have no confidence in male medical professionals when it comes to gynaecological issues. Why would I? As far as I’m concerned, the best person to understand a woman’s gynaecological pain is another woman. Pain isn’t normal and I was listened to and tended to more when women were involved in the fitting.”
Solange: 50, West Indian. Lives in South London.
“We are a very matriarchical family. In total I had nine aunties on both sides of the family, so conversations about our bodies were not taboo. We changed clothes in front of each other; we discussed any changes we noticed, so, body awareness was built into our upbringing. I think that’s where I get my confidence and sense of body autonomy from. But when I had my first Mirena coil fitted, even though my menstruation was painful and limiting my ability to work, I was still basically told “suck it up buttercup and take the pain”.
I think in health care you have to insist on being heard and getting answers and you have to do your research. Otherwise, you’ll get the bare minimum. I did my research, so I could ask specific and intelligent questions involving side effects, length of time it should remain in, and how it was supposed to help with my debilitatingly heavy periods. But among my white British friends, who go red faced at the mere mention of menopause, for example, that tenacity and agency is not typical.
In 2010 I agreed to have it done [the coil fitted] in a women’s clinic in South London where the practice nurse was a specialist in women’s health. I was accompanied by my partner. While it was painful, I’ve had two children, so I bore the pain. But make no mistake, it was not a nice experience, and it was pain worthy of note, not merely discomfort as some women are told it will be.

Five years later, the heavy bleeding started again along with some discomfort so after a referral to a private gynaecologist through my GP I had another one fitted. The pain was excruciating and though the private GP was forthcoming with information, there were no painkillers and they had to stop twice during the fitting. After a while, the time between needing to have coils replaced decreased by almost a year each time. I’m told they [doctors] are meant to check the location of the coil at least every three years during that time. I feel like I had to be the one running them down for those checks too.
The next fitting was quite the episode. I was back at home in the Caribbean, and I suspected my coil might have slipped. There was an unscheduled removal due to heavy bleeding again; one failed attempt to fit another one due to unbearable pain; taking a pill to open the cervix and finally a successful fitting two days later. No pain, no trauma; just three or four days of bleeding after.
I got lucky with the coil I had fitted last year because it was done under general anaesthetic while the surgeon was performing an exploratory procedure for endometriosis. But I specifically chose female doctors. This wasn’t always the case. I regret in the past having to rely on becoming the stereotypical angry Black woman in order for my pain to be taken seriously. Women’s pain should be believed the first time. In fact, if my partner had not accompanied me to some of those appointments and raised the alarm that I was in much more than just “some discomfort”, I fear I would have suffered in silence (as women tend to do) a lot longer. I also feel more training in terms of cultural sensitivity is required across the board in the NHS. Cultural taboos; deep rooted pre-conceived notions; language barriers and ignorance around some conditions and how they affect women of colour can all converge to make certain procedures more frightening and complex than they need to be.
“…in the Caribbean our first port of call for pain or illness is not the doctor. It is being aware of what message the body might be sending you based on your activity, and finding a herbal or natural remedy to suit.”
I’m extremely grateful for the service, but not everyone will be as body aware, forthright and refuse to take no for an answer like me. Again, I go back to my upbringing: in the Caribbean our first port of call for pain or illness is not the doctor. It is being aware of what message the body might be sending you based on your activity, and finding a herbal or natural remedy to suit. In the UK I’ve found the NHS is the starting point for body awareness, after which people take more autonomy.
I encourage women to do their own rigorous research and not to wait until the pain is at the point of passing out, or allow themselves to be shushed or patronized, to agitate for pain relief or attention before, during or after these procedures. Despite our socialization, pain is not inevitable and need not be borne silently.”
*Names have been changed to protect their privacy.
This article was written by Katrina Marshall
















